1. 5 Exercises to Avoid With a Torn Meniscus
SOURCE WordPress (live sabrinastrickland.com)
5 Exercises to Avoid With a Torn Meniscus

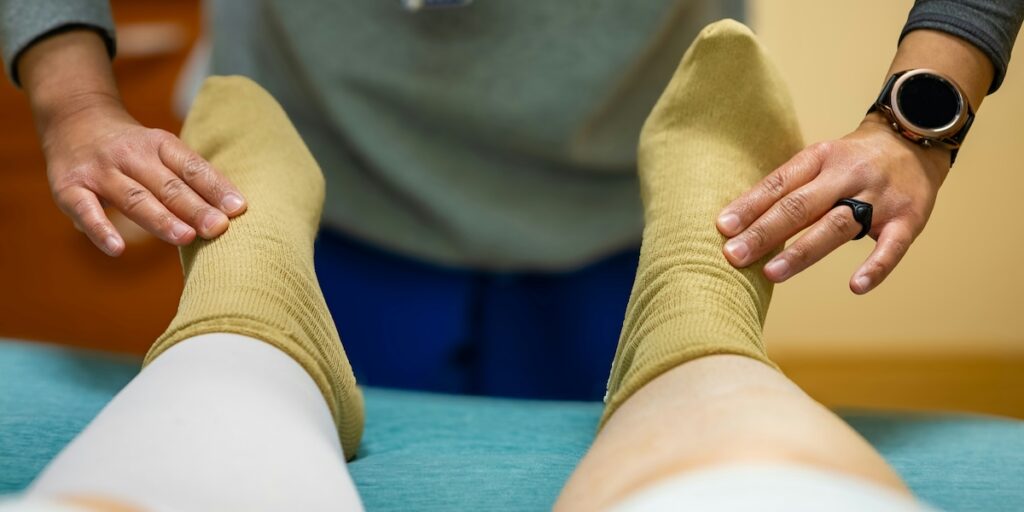
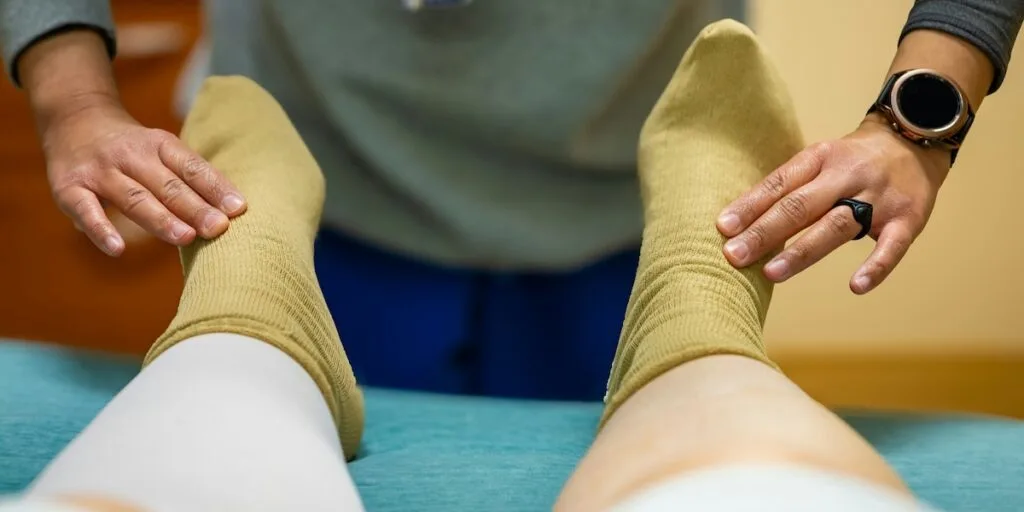
A torn meniscus is a common knee injury that can cause pain, swelling, and instability. While exercise and physical therapy are crucial for recovery, certain movements can actually worsen the injury or delay healing. Knowing which exercises to avoid is essential to protect your knee and promote optimal recovery.
Why Exercise Selection Matters
The meniscus acts as a shock absorber between your thigh bone (femur) and shin bone (tibia). When torn, it becomes vulnerable to further symptoms, especially during activities that put excessive stress on the knee joint. Repeated twisting, pivoting, or high-impact movements are common causes of meniscal tears and can aggravate an existing injury if not avoided during recovery.
Exercises and Activities to Avoid
1. Deep Squats and Lunges
Movements that require bending the knee deeply, such as full squats or lunges, put significant pressure on the meniscus. These exercises can worsen pain and increase the risk of additional tearing, especially if performed with poor form or added weight.
2. Twisting and Pivoting Movements
Sports and exercises that involve sudden changes in direction—like basketball, soccer, or tennis—are risky. These activities often require quick pivots and turns, which can catch the torn meniscus and cause further injury.
3. High-Impact Activities
Running, jumping, and plyometric exercises place repetitive, high-impact forces on the knee. These should be avoided until your knee has healed and you’ve been cleared by your physician or physical therapist.
4. Leg Extensions (Open Chain Knee Extension)
Open chain knee extension exercises, especially with resistance (such as using a leg extension machine), can strain the meniscus especially if the knee is swollen and irritate the patella and are generally not recommended during the early stages of recovery.
5. Heavy Weightlifting
Any exercise that involves heavy loading of the knee joint—such as heavy squats, deadlifts, or leg presses—should be postponed. The added force can exacerbate swelling and instability.
Safe Alternative Exercises
Instead of high-risk activities, focus on gentle range-of-motion and strengthening exercises that don’t place excessive stress on the knee. Quad sets, heel slides, and ankle pumps are some safe options during the initial phase of recovery. Often use of a stationary bike can improve symptoms.. As healing progresses, a physical therapist can guide you through a tailored program to gradually restore strength and mobility.
The Importance of Professional Guidance
Every meniscus tear is unique, and your rehabilitation plan should be individualized. Always consult with your orthopedic surgeon or physical therapist before starting or modifying your exercise routine. Ignoring pain or pushing through discomfort can lead to more serious knee problems and prolong your recovery.
Get more detailed information on meniscus injuries and recovery.
The following are additional posts to help you research your next steps:
- How To Know When You Should Have a Torn Meniscus Surgically Repaired
- Medial Meniscus Root Repair With Implantable Shock Absorber Placement
- Study on Medial Meniscus Posterior Root Tears
- Patient Information: Meniscectomy/Arthroscopy/Chondroplasty/Biopsy (PDF)
- Patient Success Story: Skier with ACL Tear and Meniscus Tear
- Patient Success Story: Medial Meniscus Tear and Arthroscopic Repair
- How Do You Know When To Take Your Knee Injury Seriously?
- Frequently Asked Questions
Photo by Gabin Vallet on Unsplash
© 2026 Dr. Sabrina Strickland MD 2012-2026. All rights reserved | Terms of Use | Privacy Policy
Functional Always active
Preferences
Statistics
Marketing
CURRENT Astro (after Tier-2 close-out)
5 Exercises to Avoid With a Torn Meniscus
Quick Summary
Certain movements consistently aggravate meniscus tears and can extend healing or worsen the injury. Deep squatting, twisting under load, lunges with rotation, jumping/plyometrics on hard surfaces, and full-depth leg presses are common offenders. The shared theme is high compressive or shearing load through a flexed, rotated knee — the position that typically causes meniscus tears in the first place. Modifying these movements protects the meniscus while you continue strengthening.

A torn meniscus is a common knee injury that can cause pain, swelling, and instability. While exercise and physical therapy are crucial for recovery, certain movements can actually worsen the injury or delay healing. Knowing which exercises to avoid is essential to protect your knee and promote optimal recovery.
Why Exercise Selection Matters
The meniscus acts as a shock absorber between your thigh bone (femur) and shin bone (tibia). When torn, it becomes vulnerable to further symptoms, especially during activities that put excessive stress on the knee joint. Repeated twisting, pivoting, or high-impact movements are common causes of meniscal tears and can aggravate an existing injury if not avoided during recovery.
Exercises and Activities to Avoid
1. Deep Squats and Lunges
Movements that require bending the knee deeply, such as full squats or lunges, put significant pressure on the meniscus. These exercises can worsen pain and increase the risk of additional tearing, especially if performed with poor form or added weight.
2. Twisting and Pivoting Movements
Sports and exercises that involve sudden changes in direction—like basketball, soccer, or tennis—are risky. These activities often require quick pivots and turns, which can catch the torn meniscus and cause further injury.
3. High-Impact Activities
Running, jumping, and plyometric exercises place repetitive, high-impact forces on the knee. These should be avoided until your knee has healed and you’ve been cleared by your physician or physical therapist.
4. Leg Extensions (Open Chain Knee Extension)
Open chain knee extension exercises, especially with resistance (such as using a leg extension machine), can strain the meniscus especially if the knee is swollen and irritate the patella and are generally not recommended during the early stages of recovery.
5. Heavy Weightlifting
Any exercise that involves heavy loading of the knee joint—such as heavy squats, deadlifts, or leg presses—should be postponed. The added force can exacerbate swelling and instability.
Safe Alternative Exercises
Instead of high-risk activities, focus on gentle range-of-motion and strengthening exercises that don’t place excessive stress on the knee. Quad sets, heel slides, and ankle pumps are some safe options during the initial phase of recovery. Often use of a stationary bike can improve symptoms.. As healing progresses, a physical therapist can guide you through a tailored program to gradually restore strength and mobility.
The Importance of Professional Guidance
Every meniscus tear is unique, and your rehabilitation plan should be individualized. Always consult with your orthopedic surgeon or physical therapist before starting or modifying your exercise routine. Ignoring pain or pushing through discomfort can lead to more serious knee problems and prolong your recovery.
Get more detailed information on meniscus injuries and recovery.
The following are additional posts to help you research your next steps:
- How To Know When You Should Have a Torn Meniscus Surgically Repaired
- Medial Meniscus Root Repair With Implantable Shock Absorber Placement
- Study on Medial Meniscus Posterior Root Tears
- Patient Information: Meniscectomy/Arthroscopy/Chondroplasty/Biopsy (PDF)
- Patient Success Story: Skier with ACL Tear and Meniscus Tear
- Patient Success Story: Medial Meniscus Tear and Arthroscopic Repair
- How Do You Know When To Take Your Knee Injury Seriously?
- Frequently Asked Questions
Photo by Gabin Vallet on Unsplash
Frequently Asked Questions
Are squats off-limits with a torn meniscus?
Not entirely — partial, controlled squats are usually fine and helpful for quad strength. What I avoid is deep squatting (where the knee bends past 90 degrees), heavy weight at the bottom, and squats with any twisting. Modifying the depth and the load, while keeping good alignment, lets most patients keep training the muscles that protect the knee without aggravating the tear.
What about deadlifts and other compound lifts?
Conventional deadlifts, done with neutral hips and knees that don't twist or buckle inward, are usually well tolerated. I often recommend hip-hinge variations, trap-bar deadlifts, and Romanian deadlifts during recovery. The key is avoiding twisting, the knees collapsing inward, and deep knee bending under heavy load. A coach can help refine your technique.
Should I stop running while my meniscus heals?
Not always. If running doesn't cause sharp pain, locking, or significant swelling, controlled mileage on flat, soft surfaces is often fine. I advise avoiding sudden cutting motions, downhill running, and high-mileage weeks during the healing phase. Cycling and pool running are excellent low-impact substitutes when regular running becomes painful.
Related Reading
- Meniscal tear / torn meniscus (specialty page)
- 6 exercises to do with a torn meniscus
- Meniscus symptoms that may self-heal
Considering treatment for a knee or shoulder concern?
Dr. Sabrina Strickland sees patients at Hospital for Special Surgery in New York City. If you would like a personalized evaluation of your symptoms and options, request a consultation below.
Book an appointment Contact the office
Enter your question below and a representative will get right back to you.
This page is not in the review queue. Want the doctor to review it?